Choose A Condition:
Please Select
FOR ADULTS WITH MODERATELY TO SEVERELY ACTIVE RA, IN COMBINATION WITH MTX
ACR20 response at Week 14 (primary endpoint): 59% of patients receiving SIMPONI ARIA® + MTX achieved ACR20 response vs 25% of patients receiving placebo + MTX (P < 0.001)1,2
At Week 14: The mean improvement from baseline in HAQ-DI* score was
0.50
for patients receiving SIMPONI ARIA® + MTX (n=395) (P<0.001)
0.19
for patients receiving placebo + MTX (n=197)1,2
ACR20 response at Week 14 (primary endpoint): 59% of patients receiving SIMPONI ARIA® + MTX achieved ACR20 response vs 25% of patients receiving placebo + MTX (P<0.001)1,2
At Week 14: The mean improvement from baseline in HAQ-DI* score was
0.50
for patients receiving SIMPONI ARIA® + MTX (n=395) (P<0.001)
0.19
for patients receiving placebo + MTX (n=197)1,2
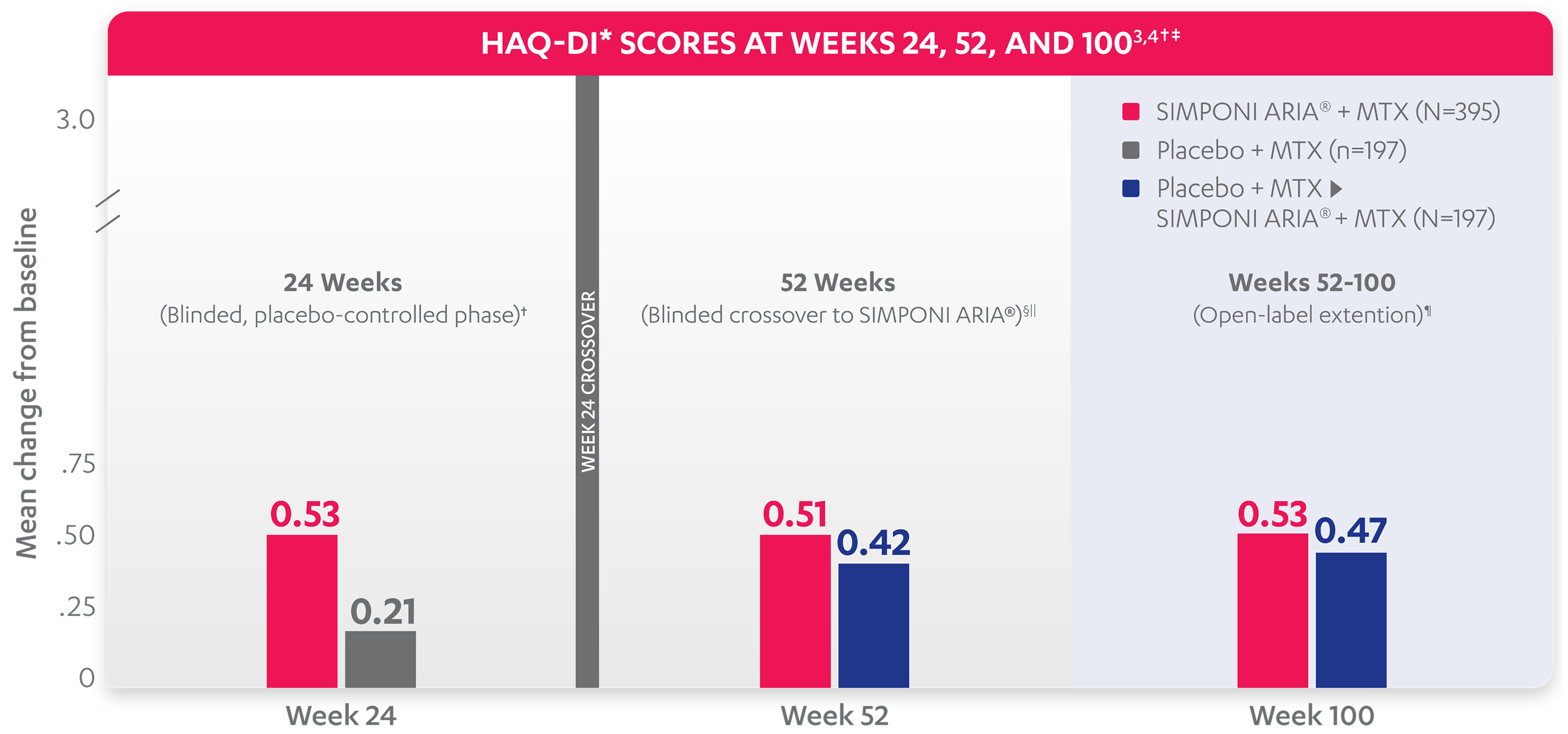
At Week 24: The mean change from baseline in HAQ-DI* score was
0.53
for patients receiving SIMPONI ARIA® + MTX (n=395)
0.21
for patients receiving placebo + MTX (n=197)1-3
WEEK 24 CROSSOVER†‡
At Week 52: The mean change from baseline in HAQ-DI* score was
0.51
for patients receiving SIMPONI ARIA® + MTX (n=395)
0.42
for patients receiving placebo who crossed over to SIMPONI ARIA® + MTX (n=197)3
OPEN-LABEL EXTENSION‡§||¶
At Week 100: The mean change from baseline in HAQ-DI* score was
0.53
for patients receiving SIMPONI ARIA® + MTX (n=395)
0.47
for patients receiving placebo who crossed over to SIMPONI ARIA® + MTX (n=197)4
HAQ-DI responses at Week 24 were not adjusted for multiplicity. Therefore, statistical significance has not been established.
Study design: GO-FURTHER™ was a global, multicenter, randomized, double-blind, placebo-controlled study in 592 adult patients who had moderately to severely active RA despite a stable dose of MTX (15-25 mg/week) for ≥3 months and who had not been previously treated with an anti-TNF agent. Moderately to severely active RA was defined as ≥6 swollen joints (out of 66 total) and ≥6 tender joints (out of 68 total), RF positive and/or anti-CCP antibody positive, and CRP ≥1.0 mg/dL. Patients were randomized to receive SIMPONI ARIA® 2 mg/kg + MTX (n=395) or placebo + MTX (n=197) as a 30-minute IV infusion at Weeks 0 and 4, and then q8w through Week 100. At Week 16, patients in the placebo + MTX group with <10% improvement from baseline in both swollen joint count and tender joint count began receiving SIMPONI ARIA® 2 mg/kg beginning with an induction regimen at Weeks 16 and 20, followed by maintenance infusions q8w in a blinded manner. At Week 24, all patients remaining in the placebo + MTX group began receiving SIMPONI ARIA® 2 mg/kg beginning with an induction regimen at Weeks 24 and 28, followed by maintenance infusions q8w in a blinded manner. All patients continued to receive MTX. The primary endpoint was the percentage of patients achieving an ACR20 response at Week 14.2
ACR20=20% improvement in American College of Rheumatology criteria; CCP=cyclic citrullinated peptide; CRP=C-reactive protein; DMARD=disease-modifying anti-rheumatic drug; HAQ-DI=health assessment questionnaire-disability index; MTX=methotrexate; q8w=every 8 weeks; RA=rheumatoid arthritis; RF=rheumatoid factor; TNF=tumor necrosis factor; vdH‑S=van der Heijde Modified Sharp score.
References: 1. SIMPONI ARIA® (golimumab) [Prescribing Information]. Horsham, PA: Johnson & Johnson. 2. Data on file. Johnson & Johnson. 3. Weinblatt ME, Bingham CO III, Mendelsohn
AM, et al. Intravenous golimumab is effective in patients with active rheumatoid arthritis despite methotrexate therapy with responses as early as week 2: results of the phase 3, randomised,
multicentre, double-blind, placebo-controlled GO-FURTHER trial. Ann Rheum Dis. 2013;72:381-389. 4. Bingham CO III, Mendelsohn AM, Kim L, et al. Arthritis Care Res (Hoboken).
2015;67(12):1627-1636.